Eczema in children: everything you need to know

It itches and can even make your children a bit irritable: no one wants their child to have to deal with eczema. A basic understanding of the condition, however, will reveal just how common it is but also that treatments can help improve outcomes. The first approach to fight against eczema is to develop your understanding of the disease and to bust certain myths.
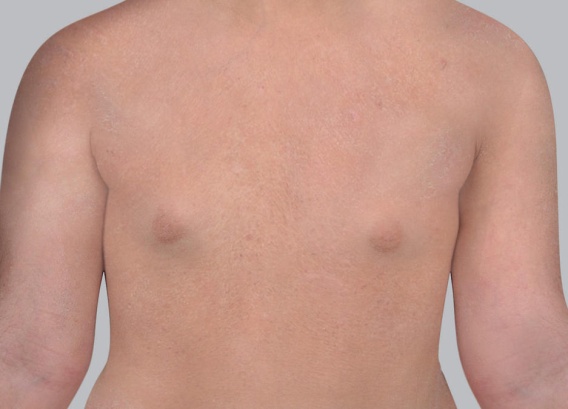
What does eczema in children look like?
There are several different types of eczema, but atopic eczema is the most common, so we will start there.
Atopic eczema in children
Atopic eczema is also known as atopic dermatitis. Both terms refer to the same condition. Let’s start with its characteristics.
- Dry or very dry skin
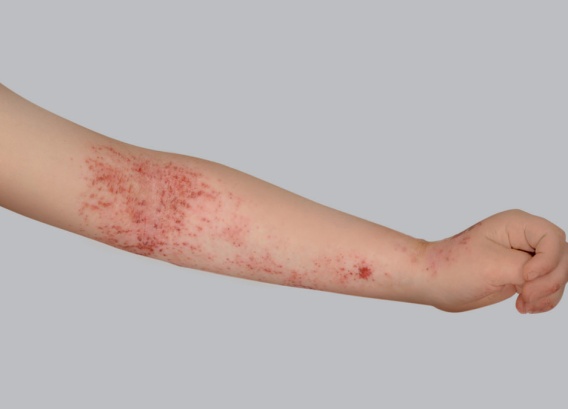
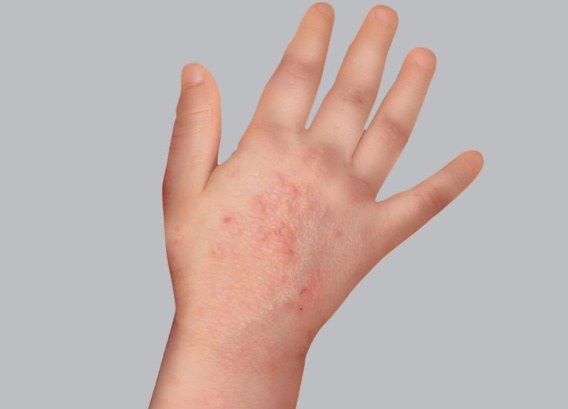
- Red patches
- Itching
- Oozing
- Thickening of the skin
- Marks from scratching
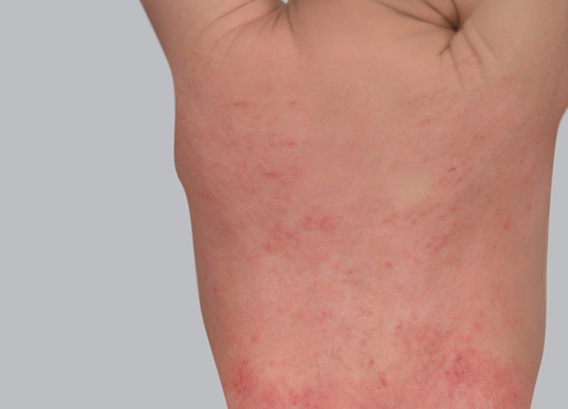
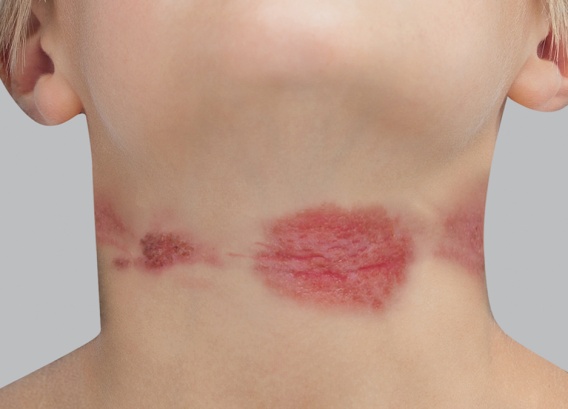
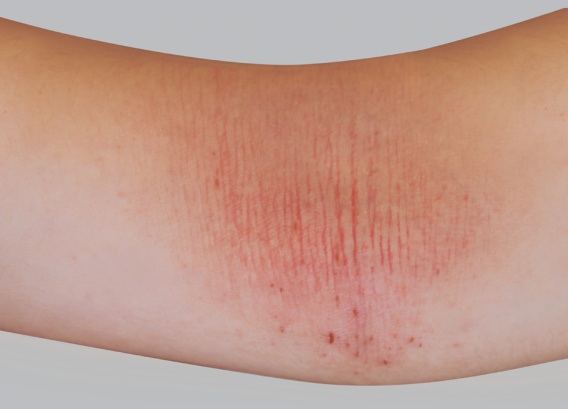
Red patches appear and can quickly become covered in little vesicles. They then ooze, which causes scabs to form when this fluid dries. All throughout this progression, the eczema patches itch and produce an overwhelming urge to scratch. Fortunately, flare-ups are followed by periods of remission: atopic eczema presents in alternating periods of flare-ups and remission.
Over time, eczema flare-ups are likely to become less frequent. In all likelihood, your child’s eczema will go away by the time they are a teenager, but it could continue into adulthood.
In children with atopy, eczema patches most often appear in the folds of the elbows and knees and on the wrists and ankles, but other areas of the body can also be affected.
There is no cure for atopic eczema, which means you cannot prevent flare-ups from coming back. But you can provide suitable treatment for flare-ups. Indeed, you can treat eczema in order to provide soothing relief and even reduce the frequency of flare-ups.
Treatments
Treat it as fast as possible:
The sooner you act, the better your chances of alleviating and delaying the onset of the next flare-up.
Treatments:
A combination of two treatments is used to reduce the frequency and severity of atopic dermatitis flare-ups.

Cortisone cream
Emollient skin care
Adjusting your daily habits
There are a thousand little things you can do to improve life with atopic eczema and reduce flare-ups. Tips on how to scratch less, simple ways to talk about it at school, or things you should avoid doing and activities you can absolutely enjoy if you take the proper precautions!
Atopic eczema is caused by a malfunction in the skin and in the defense mechanisms: your child has atopic skin. Atopic skin is more porous than normal skin and is thus unable to act as a proper barrier. What is more, it is abnormally reactive to its environment... This causes red patches to appear, along with itchy flare-ups.
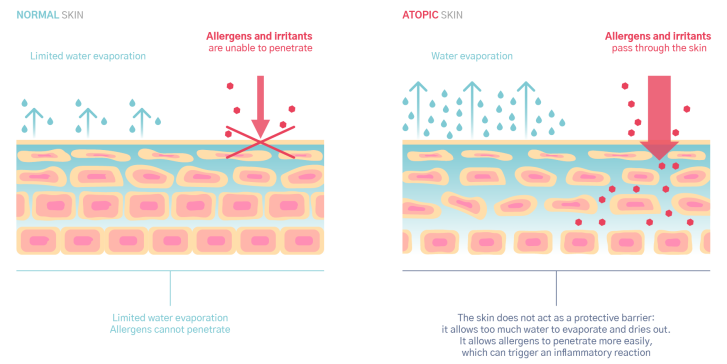
Inflammation is triggered by a combination of environmental factors, allergens, irritants, microbes, scratching, overheating, etc.
This hypersensitivity to the environment, known as atopy, is hereditary and thus runs in the family.
Atopic eczema is a sign that your child has atopy, which means their skin is hypersensitive to the environment. They could, therefore, develop other manifestations of atopy, such as asthma. Symptoms of asthma include nighttime coughing, wheezing or shortness of breath during physical activity.
Other forms of atopy:
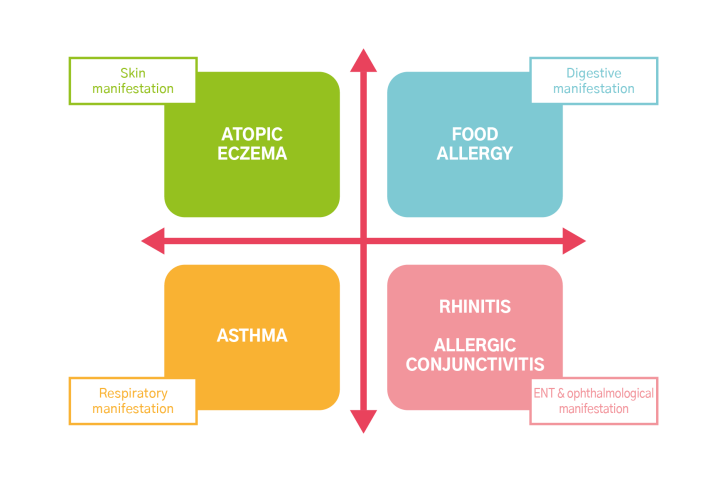
Contact eczema in children
An allergic reaction
Although atopic eczema is by far the most common, there is another type of eczema known as allergic contact eczema. This type of eczema differs from atopic eczema in terms of its onset. It is an allergic reaction that occurs when the skin comes into contact with a given substance: costume jewelry or a shower gel, for example.
Solutions and treatments
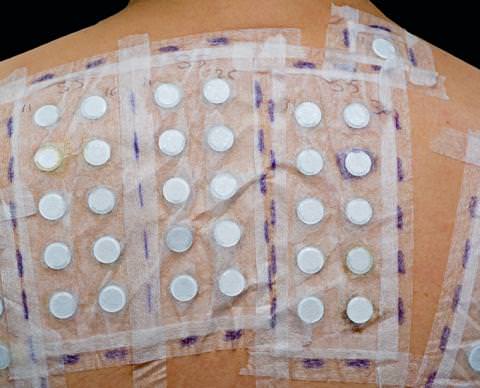
Eczema is treated with topical corticosteroids. To prevent recurrence, however, you must identify the triggering allergen so that you can avoid it in the future. Some simple questions can sometimes help to identify the allergen, but allergy tests do a better job of unveiling the culprit.