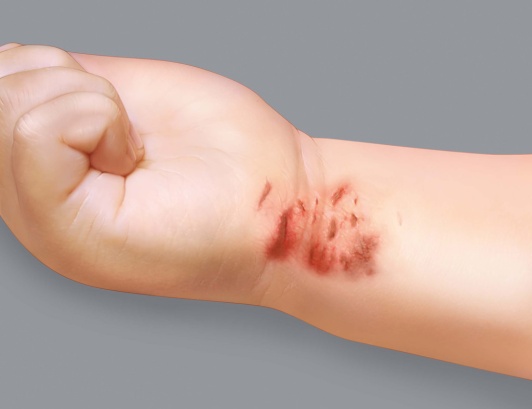
What is atopic eczema?

The main symptoms of atopic eczema are itchy red patches and dry skin. Another distinctive sign is alternating periods of flare-ups and remission.
In most cases, this type of eczema appears in childhood and usually subsides by adulthood.
Atopic eczema is not contagious; you cannot “catch it”! In simple terms, it means that the skin becomes inflamed easily. This is why it is also known as atopic dermatitis.
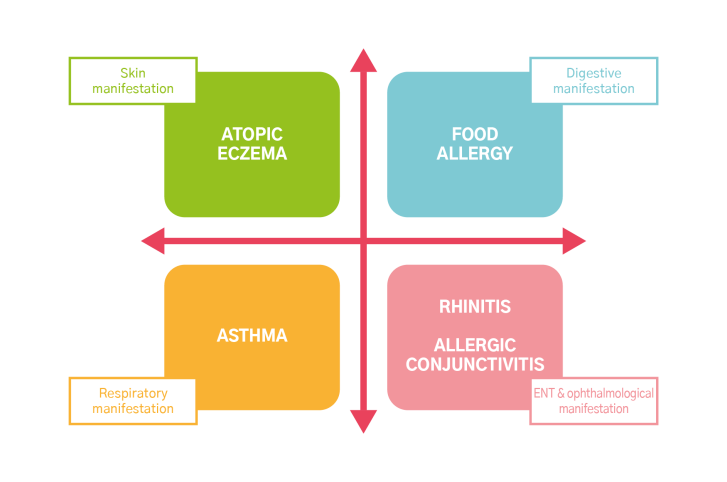
Atopic eczema is the skin manifestation of atopy, just as asthma is its respiratory manifestation.
Recognizing atopic eczema
A chronic disease
We often talk about “eczema flare-ups” because this condition is chronic. Eczema flare-ups are followed by periods of remission, during which patients can even forget they have the disease... until the next flare-up.
Atopic eczema is hereditary and thus differs from contact eczema which is acquired and can be treated simply by avoiding the triggering agent.
Atopic eczema symptoms
Below are the symptoms of atopic eczema, also known as atopic dermatitis:
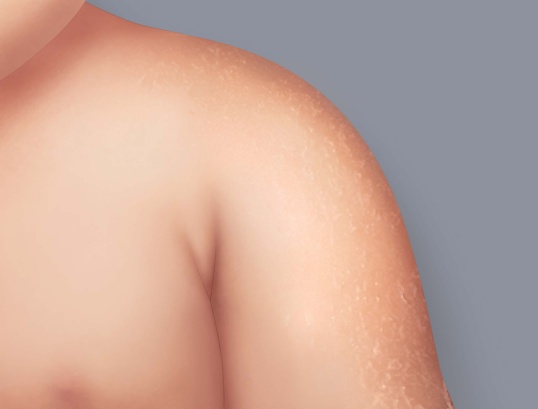
- dry to very dry skin
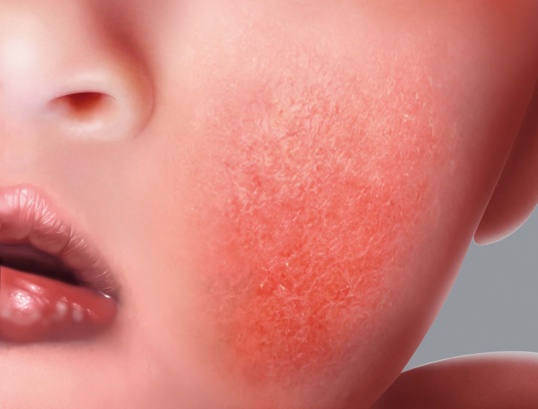
- Red patches
- Itching
- Oozing
- Thickening of the skin (lichenification)
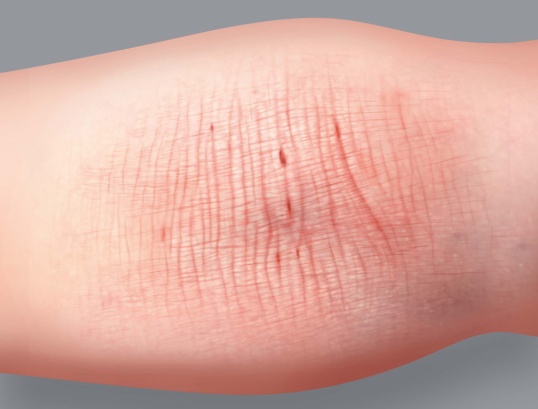
- Marks from scratching (excoriation)
Flare-up symptoms are always accompanied by severe itching which impedes sleep and causes irritability.
During remission phases, skin remains dry and tight, even to the point of itching.
The severity of symptoms varies greatly from one person to the next, but inflammation always develops in the same order: erythema (redness) with possible edema (swelling) > vesicles (little blisters) > oozing (from blisters opening) > scabs
A mobile app is available to help you assess the severity and evolution of your eczema over time
It is impossible to “treat” atopic eczema so that it goes away completely, as you would a toothache for example. However, effective treatments are available, and, with the proper follow up, they soothe itching, treat flare-ups and reduce their frequency.
How does the condition evolve over time?
For most people, the severity and frequency of flare-ups diminish over time until they go away completely by the time they reach adulthood.
Areas of the body affected
Atopic eczema appears on different areas of the body depending on the person’s age. So, what is the most common place for patches and redness to appear?
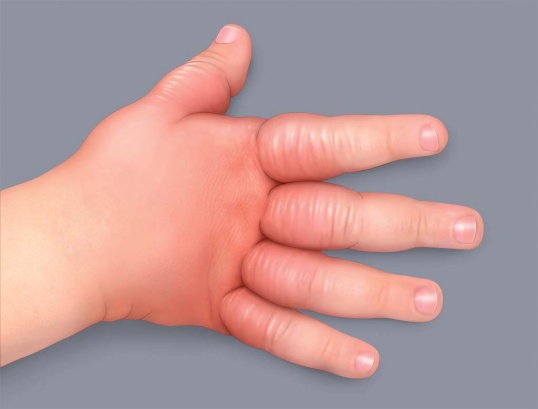
In babies, atopic eczema affects plump areas (cheeks, forehead), the arms and the stomach.
Atopic eczema appears in the folds of the elbows and knees and on the hands and face (around the mouth, eyelids, behind the ears).
In the majority of cases, atopic eczema tends to disappear in adolescence.
If atopic dermatitis persists into the adult years, patches may appear anywhere on the body, but especially on the face, neck and hands.
WHAT IS THE DIFFERENCE BETWEEN ATOPIC ECZEMA AND ATOPIC DERMATITIS?
There is none. The two terms refer to exactly the same condition. However, when the terms eczema, atopy and dermatitis are used alone, they have very different and much broader meanings.
- Eczema: skin inflammation associated with itching
- Atopy: genetic condition causing hypersensitivity to the environment
- Dermatitis: skin inflammation
The causes of atopic eczema
There is a lot of information surrounding atopic eczema. Fortunately, science has made great strides in this area, and we are beginning to better understand this disease.
It is important to distinguish the cause from the triggering factors.
What causes atopic eczema?
- An atopic predisposition is caused by genetic factors which impact both the skin’s structure and its defensive responses to the environment.
- On atopic skin, flare-ups are triggered by environmental factors.
 Genetic predisposition
Genetic predisposition
 Sensitivity to the environment
Sensitivity to the environment
 Atopic predisposition
Atopic predisposition
The underlying cause: atopic skin
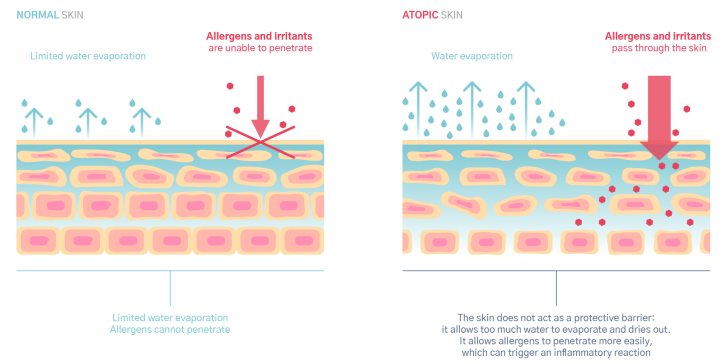
Human skin acts as a barrier. It blocks UV rays, pollution particles, allergens and even chlorine in the pool, and more. In short, it protects you. Atopic skin, however, is more fragile and unable to function correctly. It has two major malfunctions which combine and lead to the all-too-familiar symptoms of redness and itching.
Atopic skin is no longer able to act as a barrier and becomes more permeable to irritants and allergens in the environment, making it easier for harmful elements to penetrate the skin.
Atopic skin is also hypersensitive to its environment. As a result, when allergens or irritants penetrate the surface, skin becomes inflamed very easily.
Skin becomes inflamed due to its excessive immune response. In fact, people with atopy overproduce antibodies called Immunoglobulin E (IgE), making them more reactive to allergens. However, atopic eczema is not technically an allergy.
ATOPIC SKIN: VERY DRY SKIN
Because atopic skin is more permeable, it also loses more water through evaporation. As a result, it becomes very dry. That is one reason why hydrating skin care helps sooth eczema.
Atopic skin is hypersensitive to the environment and to the different allergens found within this environment. This predisposition to over-react to the environment is hereditary.
RISK OF 50% IF ONE PARENT IS AFFECTED
Atopy can manifest in different ways. Some people have asthma, some hay fever, and others eczema... Atopic manifestations tend to appear in the same person in a precise sequence. This phenomenon is known as the “Atopic March”.
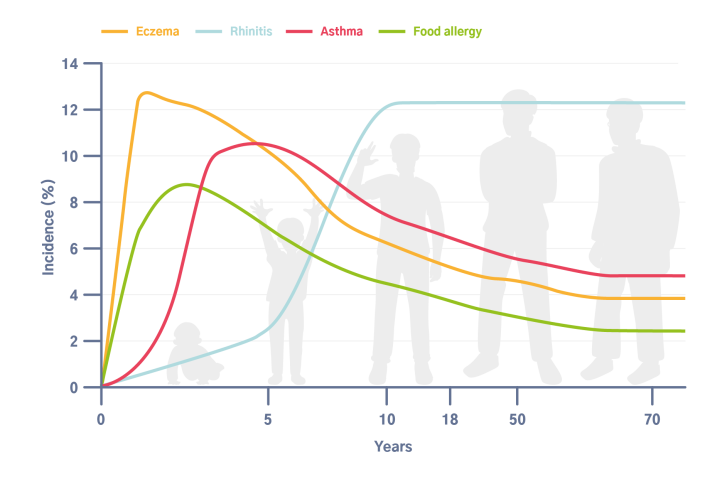
Triggering and aggravating factors
We can better anticipate flare-ups by improving our understanding of their triggering and aggravating factors. That said, a complex combination of factors is usually involved and can be difficult to identify. The factors below are suspected to contribute, one way or another, to the onset of flare-ups (note that opinions vary within the scientific community):
- climate
- pollution
- temperature variations
- certain clothing
- sweat
- certain foods
- stress
- allergens
- microbes
- scratching
Who is affected by atopic eczema?
Children are the most affected
Generally speaking, atopic eczema has a very early onset, occurring before the age of three months on average. Given the fact that it usually goes away within a few years, children are the most affected group. And at an increasing rate!
1 IN 5 CHILDREN UNDER THE AGE OF 7 IS AFFECTED
A public health problem throughout the industrialized world
The number of atopic eczema cases has tripled over the last 30 years. More and more people are affected, especially in industrialized countries and even more so in cities.
What is behind this rapid increase? Firstly, the presence of multiple aggravating factors, such as pollution, in modern, urban environments.
In addition, excessive cleanliness and our increasingly “sanitized” environments probably contribute to this increase.
How does living in a sanitized environment contribute to allergies? Although the immune system is rarely called upon to fight off infections in such an environment, it may over-react to certain allergens.