Eczema in infants: everything you need to know

Are dry skin and red patches causing baby to fuss? It might well be eczema. But there is no need to turn your daily life upside down to soothe baby. Sometimes, a simple adjustment in your daily habits and care is all it takes. Once the doctor has confirmed the diagnosis, simple products can be used to provide comfort.
Atopic eczema in infants
Atopic eczema is the most common form of eczema. Its onset often occurs within the first few months of life, thus affecting infants. This type of eczema is associated with skin which fails to protect itself from the environment and has inflammatory reactions. It is not contagious!
Recognizing this type of eczema
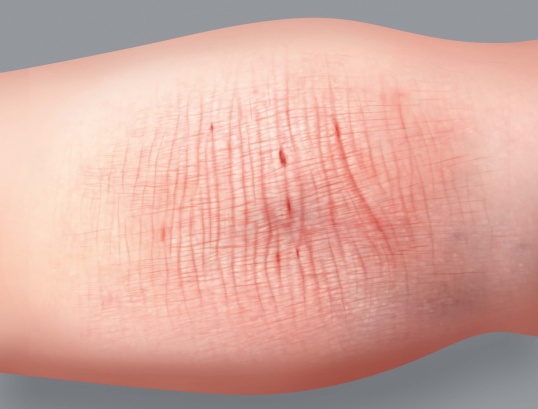
- Dry or very dry skin
- Red patches
- Itching
- Oozing
- Thickening of the skin
- Marks from scratching
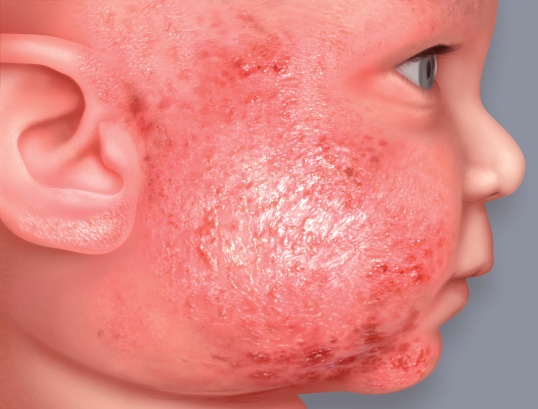
Red patches become covered in little vesicles which tend to ooze and ultimately form scabs.
Parents sometimes confuse eczema with urticaria or vice versa. The two are easy to distinguish, however: the red patches resulting from urticaria move around and do not ooze.
This type of eczema has an important characteristic: alternating periods of flare-ups and remission. Treating flare-ups with a topical corticosteroid is important to speed up the healing process.
In most cases, flare-ups will gradually become less frequent and severe, before going away entirely after a few years. In some cases, however, atopic dermatitis continues into the adult years.
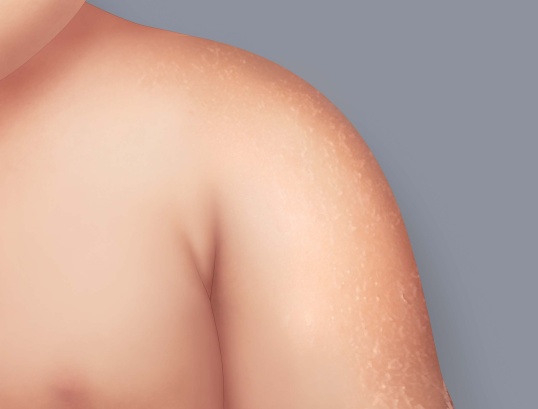
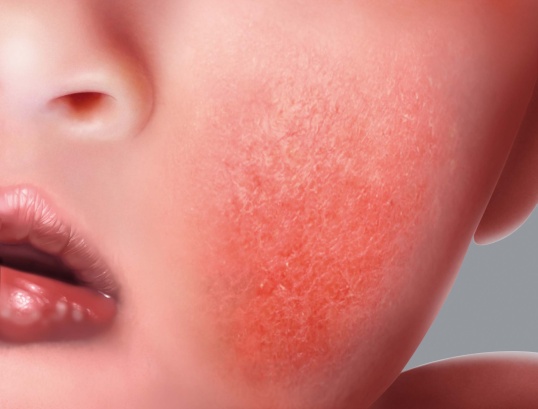
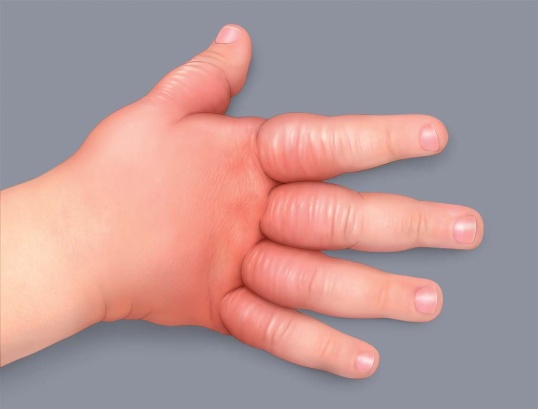
In infants, redness appears mainly on the face (cheeks and forehead), arms, legs and stomach.
Eczema on the face
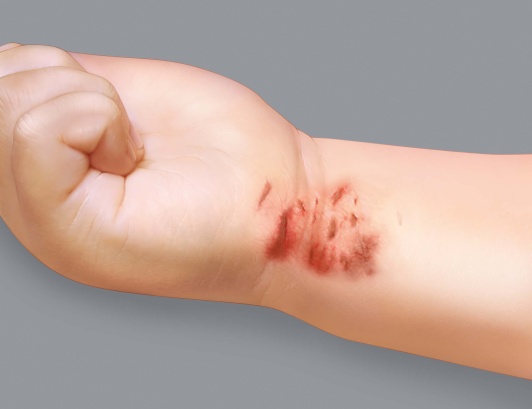
Eczema on the arms
Eczema on the stomach
Eczema on the legs
Why does my baby have atopic eczema?
Your baby has what we call “atopic skin”. This means his often dry to very dry skin is unable to act as a proper protective barrier. External molecules are able to pass through the skin, which becomes inflamed easily. As a result, redness and itching occur.
Atopic eczema is hereditary and linked to a malfunction in both the skin and the defense mechanisms, presenting as hypersensitivity to the environment. However, it is not an allergy.
Atopy-prone skin is hereditary. Often times, it already affects others in the family. Atopic eczema is triggered, however, by a combination of external factors, such as pollution, climate, sun exposure, and more.
 Genetic predisposition
Genetic predisposition
 Sensitivity to the environment
Sensitivity to the environment
 Atopic predisposition
Atopic predisposition
How to provide your baby with soothing relief from atopic eczema
Eczema in infants cannot be cured with a treatment to simply make it go away. You can, however, reduce the severity and delay the onset of the next flare-up.
Skin care
The sooner you treat atopic eczema in infants, the sooner it is likely to go away. But there’s more: studies show that you also reduce the risk of developing allergies.
It all starts with very dry skin. If your baby has never had eczema but has very dry skin, applying an emollient to their skin every day will increase your chances of reducing the risk of atopic eczema.
A combination of two types of treatments is often used to relieve atopic eczema.
Corticosteroid-based cream
Emollient skin care (hydrating)
Everyday soothing habits
Avoid overly hot baths, opt for an ultra-rich soap, towel dry baby by dabbing rather than rubbing the skin, regulate the temperature in baby’s room, etc. A whole range of habits can go a long way to provide soothing relief for baby.
Contact eczema in infants
An allergic reaction
This type of eczema should not be confused with atopic eczema. It is a skin allergy to a given substance found in a product or object: cosmetic or cleanser, costume jewelry, etc. Although rarer in adults, it can be observed in infants.
Solutions and treatments
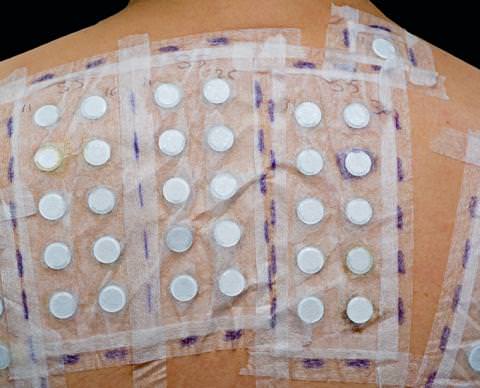
The goal is to identify the triggering allergen so that it can be avoided. To this end, we explore the areas affected by eczema and the products that have come into contact with the skin. Allergy tests may be conducted to identify the triggering agent.