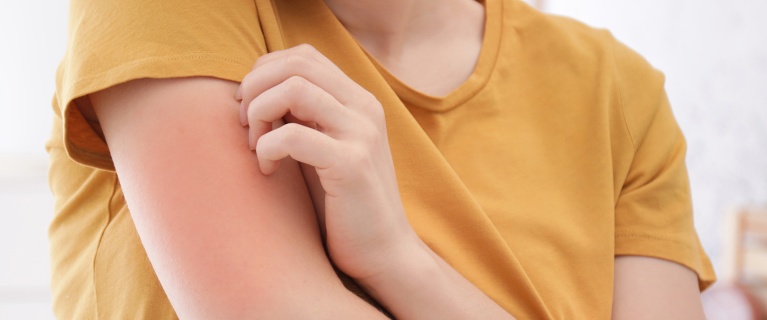

What is red skin syndrome or "burning" skin?

As with all treatments, topical corticosteroids must be used properly: you should not seek to increase doses for greater efficacy or use them inappropriately. Among the effects observed in cases of misuse is red skin syndrome, which remains controversial.
What is red skin syndrome?
It is likely to be related to abnormal use of topical corticosteroids, either in an abusive or inappropriate manner.
The most common symptoms are:
- redness is the almost constant sign
- papules & pustules ("pimples" resembling acne)
- burning sensations
- tingling
- itching
- swelling
- dry and/or peeling skin
- pain
- facial flushing amplified by heat or the sun
It mainly affects women
In fact, 85% of cases are in women. Under what conditions did these women report having used topical corticosteroids? Almost systematically, topical corticosteroids were applied to the face (97% of cases) either for atopic eczema or for other reasons (desire to lighten the skin, acne, rosacea, etc.).
This syndrome is never observed during treatment but may be observed when topical corticosteroid use is discontinued, always in patients who have used them over a very long period (several months of daily use).
A rare and controversial complication
This topical corticosteroid discontinuation syndrome after addiction is not only very rare but also not universally accepted: its existence is not yet agreed upon in the scientific community. In fact, most of the studies that refer to it have a low scientific value, according to the latest review carried out by specialists, who are waiting for other studies to clarify matters.
This side effect does not occur during normal use.
Topical corticosteroids are generally well tolerated when the treatment indications are respected for eczema, psoriasis, or other bullous diseases.
Two types of abnormal use may be related to this syndrome:
- Abusive: too much product or too often
- Inappropriate: use on other inflammatory dermatoses such as acne or rosacea.
What should you do if you suspect "red skin"?
The first thing to do is to turn to a specialist dermatologist because red skin syndrome should not be confused with an eczema flare-up, a contact allergy, or even a skin infection (one of the complications of eczema).
If it is indeed a rash that has occurred after prolonged treatment with cortisone cream that has been discontinued, your doctor will probably indicate an alternative treatment to topical corticosteroids and may recommend cool water compresses, which calm inflammation, as well as possible psychological support.
Should you avoid topical corticosteroids?
Not at all, you can use them with peace of mind. Of course, you have to learn how to use them properly: they are the most effective and risk-free first-line treatment.
Why do we think they cause swelling?
This is a side effect seen when cortisone is taken orally or injected, at much higher doses, which can cause puffiness.
Why do we think they are addictive?
If the correctly applied topical corticosteroid no longer seems to work, even though it was effective at the beginning of treatment, it is either that:
- the cream used is inappropriate (topical corticosteroid not powerful enough)
- the cream is used incorrectly, often in too small a quantity (we often use too little, think of the fingertip rule).
Although they come in the form of a cream, topical corticosteroids are still a drug: the dose and frequency of application must be respected. They are certainly a little restrictive and require great regularity of use, but this regularity leads to a real improvement in quality of life.

